Why should you receive
organ transplantation in AMC?
Organ transplantation is an operation that replaces the affected organ of a terminally ill patient with a healthy organ of a brain-dead or a living person. Transplantation is performed on a patient who cannot be treated with conventional therapies due to intractable diseases. Transplantation of organs including the solid organs such as the kidney, liver, pancreas, heart, and lungs as well as the tissues such as the cornea, bone marrow, bones, blood vessels, cartilage, amnions, fasciae, and heart valves are possible. After the first successful kidney transplantation in 1969, transplantation of the kidney, cornea, and bone marrow has been performed. Thereafter, the first deceased donor liver transplantation (DDLT) in 1988 was succeeded by the pancreatic and heart transplantations in 1992 and the lung transplantation in 1996.
AMC’s Liver Transplantation Center laid the foundation stone for DDLTs in Korea and paved the way for raising awareness for brain dead organ donation and transplantation. In May 1992, the center began with the first deceased donor multi-organ transplantation. The center had received global attention as it was the first to perform living donor liver transplantation using a modified right lobe graft in 1999, a dual living donor liver transplantation in 2000, and exchange liver transplantation in 2003. Furthermore, a steady stream of overseas medical professionals from prestigious transplantation centers around the world has been visiting AMC for training.
AMC’s Liver Transplantation Center, with disregard to the number of surgeries, has strengthened its outstanding position in treatment outcomes and survival rates for each type of organ transplantation; all the meanwhile, strengthening its efforts in continuous research and experiments and advanced training programs. The center will strive to concentrate on treatment, research, and training to achieve increased survival rates and better treatment outcomes.
Treatment Method

Liver transplantation
The liver is a vital organ for maintaining life. Its functions are so diverse and complex that there is no artificial device that can replace it. Therefore, the only way to treat patients with end-stage liver diseases is liver transplantation. Liver transplantation is a surgical procedure that removes the afflicted liver and replaces it with a healthy one. Liver transplantation first began in the United States in 1963, followed by Korea in 1988, and by AMC in 1992. AMC had succeeded the first pediatric living donor liver transplantation in 1994, and the first adult living donor partial liver transplantation in 1997. Since then, AMC has been actively performing liver transplantations.
-
Recipient
Adult patients with end-stage liver diseases such as liver cirrhosis, liver cancer and acute fulminant hepatic failures and pediatric patients with congenital liver cirrhosis, biliary atresia, and metabolic liver diseases are all indications for liver transplantation. Whether or not recipients are good candidates for liver transplantation is determined by examining and analyzing each patient’s medical condition and characteristics.
-
Donor
The liver is an organ that can be transplanted in part or in whole. Patients can receive a portion of the liver from family members or a whole liver from brain dead patients. The donor’s remaining liver regenerates, allowing for the donor to lead a normal healthy life without risks. A donor and recipient must be of similar build, and possibility for donation is determined after thorough examinations. A donor whose liver functions are normal and healthy is qualified as a donor candidate as long as the liver is without illness, infection, and cancer. If the blood type of the donor and the recipient is incompatible, preoperative therapeutic plasma exchange may be done.
-
Transplant procedure
1) Living donor transplantation (partial transplantation)
- Recipient examinations (General Surgery or Pediatric Department Outpatient Clinic)
- Donor examinations (General Surgery Department Outpatient Clinic)
- Check if transplant is possible and hospitalize
- Hospitalize and perform a thorough examination(transplant cancelled if there are abnormal results)
- Review the results and perform liver transplantation
2) Care after transplantation
Patients will stay in the hospital for around three to five weeks after liver transplantation and will have regular outpatient visits after discharge. To prevent complications of organ transplantation, all patients must take an immunosuppressant drug every day. Also, patients who had hepatitis B before liver transplantation regular injections of hepatitis B antibodies will be given to prevent hepatitis B relapse after surgery.
AMC's treatment performance
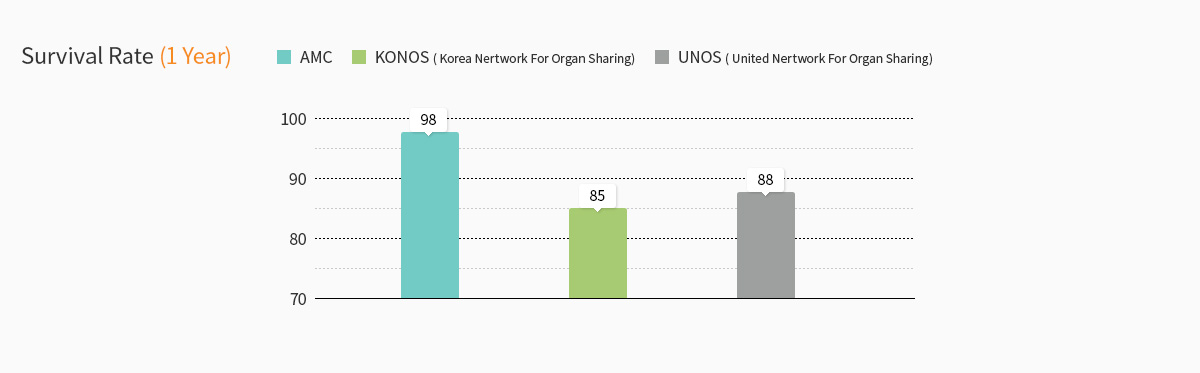
AMC’s Liver Transplantation Center laid the foundation stone for DDLTs in Korea and paved the way for raising awareness for brain dead organ donation and transplantation. In May 1992, the center completed the first deceased donor multi-organ transplantation. In July 1992, the Center succeeded Korea’s first simultaneous pancreas-kidney transplantation. Then in August 1992, it completed the first liver transplantation and then the first heart transplantation in November. Ultimately, it took a lead in the field of deceased donor organ transplantation.
Moreover, the center performed Korea’s first living donor partial liver transplantation in 1994, the first simultaneous liver-kidney transplantation in 1999, the first adult-to-adult split-liver transplantation in 2003, the first simultaneous heart-kidney transplantation in 2005, and the first living donor simultaneous kidney-pancreas partial transplantation in 2006. It also performed the first simultaneous liver-heart transplantation in 2007, the first simultaneous seven-organ multi visceral transplantation in 2011, the first simultaneous liver-lung transplantation in 2012, and the first simultaneous liver-heart-lung transplantation in 2015. Such performance has contributed greatly to enhancing Korea’s overall medical skills and expertise in organ transplantation. Not only that but also, the center had received global attention as it was the first to perform living donor liver transplantation using a modified right lobe graft in 1999, a dual living donor liver transplantation in 2000, and exchange liver transplantation in 2003.
Thanks to recent corneal transplantation, bone marrow transplantation, and tissue transplantation, many patients have been given new hope. Every transplantation team at the center makes continuous efforts in attaining remarkable achievements. Through their efforts, achievements such as 9,000 liver transplantations by April 2025, 7,000 kidney transplantations by December 2022, 900 heart transplantations by August 2023, and 500 pancreas transplantations by October 2022 were made possible.
