Why should you receive treatment
for pituitary disorders in AMC?
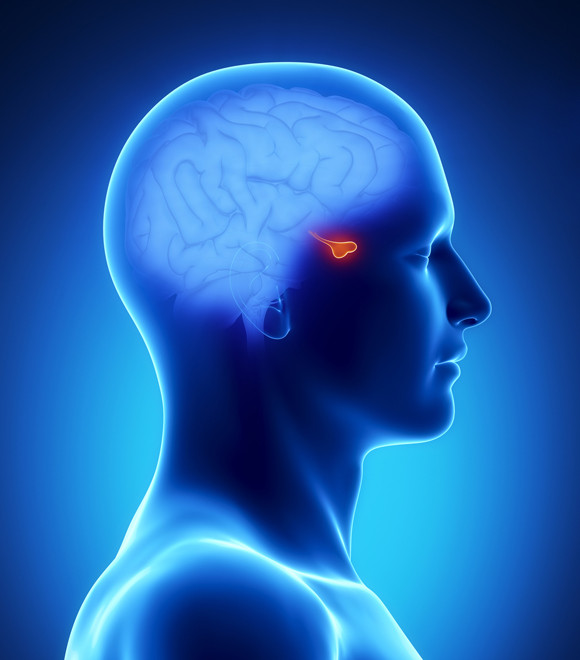
The pituitary gland located in the sella turcica, which resembles a saddle, is anatomically divided into the adenohypophysis (anterior pituitary) and the neurohypophysis (posterior pituitary). It connects to the hypothalamus of the brain which engages in the secretion and control of the hormones in the body. The pituitary gland is also surrounded by the optic nerve, the optic chiasm, the internal carotid artery, the cavernous sinus, and the temporal lobe, leading to various related symptoms if a tumor develops.
Pituitary gland tumors can cause hyperpituitarism, such as galactorrhea, gigantism or acromegaly. They may also cause panhypopitutarism (also called Simmonds’ disease), dwarfism, microsomia, diabetes insipidus or syndrome of inappropriate antidiuretic hormone secretion (SIADH). For instance, prolactin-producing adenomas (also called prolactinomas) are the most common benign tumors of the pituitary gland and account for 40% of pituitary adenomas. Prolactinomas mostly affect women in their 20s and 30s, yet the reason is unknown.
The Pituitary Clinic at Asan Medical Center offers fast-track services for the diagnosis and treatment of patients with pituitary disorders. Specialists in endocrinology and metabolism, neurosurgery, and radiation oncology collaborate in sharing opinions to accurately and rapidly decide on optimal therapy and to treat the patients accordingly.
The department of endocrinology and metabolism offers drug therapy and work together with the department of neurosurgery for patients who require surgery to provide preoperative preparations, diagnosis, postoperative care, and drug therapy.
Treatment options

Treatment options for pituitary tumors mainly include drug therapy, surgery, and radiation therapy. If a large-sized non-functioning tumor causes visual impairment or exerts pressure on surrounding organs, surgical removal is readily necessary. In contrast, in the case of microadenomas, treatment is not necessarily required. Without any evidence of pressure symptoms of surrounding organs or hypersecretion of hormones, the non-functioning pituitary adenoma such as the gonadotropin secreting pituitary microadenoma, only need regular hormone screenings and imaging. In the case of large-sized adenomas or growing microadenomas, treatment is necessary if infertility, discomfort of breast milk secretion, amenorrhea, gynecomastia, decreased testosterone, osteoporosis and hirsutism are observed.
Drug therapy
Drug therapy is based on the principle that the hypothalamic peptide controls the biosynthesis and release of pituitary hormones. Currently available drugs include dopamine receptor agonists. for the treatment of prolactinoma and somatostatin analogues for the treatment of acromegaly. According to recent studies reported so far, combined therapy is the most desirable approach.
Surgery
The surgical indications for pituitary disorders include non-functioning adenomas causing neurological symptoms like visual impairment or visual field defects and some functioning tumors such as growth hormone-producing adenomas (i.e. acromegaly) and adrenocorticotropic hormone-producing adenomas (i.e. Cushing’s disease). The purpose of the surgery is to relieve compressing pressure to the optic and oculomotor nerves or to remove hormone-producing tumor cells totally.
The most common surgical treatment methods for pituitary adenomas have been microscopic or endoscopic transsphenoidal surgery through the nostrils. Since the pituitary gland is located at the bottom of the brain, a tiny hole is made inside the nose to access the pituitary gland to get rid of the tumor. Removing the tumor prevents the aggravation of neurological deficit caused by the growing tumor. This approach is easier and safer to perform than craniotomy; therefore this method is frequently used to remove most pituitary adenomas. The endoscopic surgery, especially, is a new technique for pituitary diseases that can provide a panoramic view and high resolution images of the pituitary gland, tumors, and their adjacent neurovascular structures.
The patient receives the preoperative evaluations by a neurosurgeon, endocrinologist, ophthalmologist, and rhinologist; they compose the multidisciplinary team for pituitary tumors. The patient undergoes a transsphenoidal surgery for about 3 hours and can leave the hospital 3 days after the surgery if they do not show any post-surgical complications like cerebrospinal fluid leakage or postoperative infections. AMC’s pituitary surgery team completes more than 150 cases of pituitary surgeries annually.

Radiation therapy
Radiation therapy is usually considered when surgery or drug therapy fails or when there is recurrence. There are two forms of radiation therapy, i.e. fractionated radiation therapy and stereotactic radiosurgery (SRS). The former is a conventional method of radiation therapy in which multiple, small, daily doses of radiation are delivered usually for five to six weeks, whereas the latter is a newer technique featuring a delivery of high-precision high dose radiation during a single or up to five sessions. With the advent of sophisticated imaging and targeting techniques, SRS offers a higher chance of cure or tumor control and greater safety as well as patient convenience.
AMC prides in its comprehensive SRS service for it is equipped with the cutting-edge radiosurgery systems, the Gamma Knife Icon, and the CyberKnife Version 9.5. Since the first introduction of the Gamma Knife in Asia in 1990, more than 8,000 Gamma Knife treatments have been conducted. In 2011, the CyberKnife system was introduced, which is used for tumors that are difficult to treat with the Gamma Knife. The Gamma Knife and CyberKnife are used in a complementary fashion depending on each patient’s specific conditions to achieve the best results.
Treatment outcomes
Immediate surgery reduces pressure and restores visual impairment of up to 90%. Some of the hypopituitarism improves as well. Radiation therapy will lower the possibility of a recurrence, but adverse effects may occur such as hypopituitarism, damage to the optic nerve, neuropsychiatric effects, and the possibility of secondary tumor development due to irradiation.
This treatment may be applied if a patient does not respond to drug therapy or continuously suffers from visual impairment. Depending on the doctor’s skills, it is reported that the success rate is 80-90% in microadenomas and less than 50% in large-sized adenomas.
